| Table of Contents |  |
|
Original Article
| ||||||
| Postoperative analgesia in laparoscopic liver resection: An international survey | ||||||
| Manu-Priya Sharma1, Georgina Cubas1, Simon Cottam2, James Gill1, Gudrun Kunst3, Zoka Milan4 | ||||||
|
1Locum Consultant Anesthetist, King's College Hospital, London, UK.
2Clinical director of Anesthesia, King's College Hospital, London, UK. 3Consultant Anesthetist, Research Clinical Lead, Reader in cardiac anesthesia, King's College Hospital, London, UK. 4Consultant Anesthetist, Honorary Senior Lecturer, Visiting Professor, King's College Hospital, London, UK. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Manu-Priya S, Cubas G, Cottam S, Gill J, Kunst G, Milan Z. Postoperative analgesia in laparoscopic liver resection: An international survey. Edorium J Anesth 2016;2:14–19. |
|
Abstract
|
|
Aims:
We undertook a worldwide survey of current practices regarding postoperative analgesic management of laparoscopic hepatic resection (LHR).
Methods: An online 10-question survey was sent to hepatobiliary units worldwide. Results: Forty-five responses were received. Anticipated postoperative pain was described as "less intense" in LHR when compared to open hepatic resection (OHR) in 41/45 centers and "equally intense" in 3/45, and "more intense" in 1/45. Only 2/45 respondents thought that the pain score was lower than 2. Most of the responses (11/45) indicated VAS 4, while all the scores above 4 were represented equally. Overall, 2/5 of the centres used the same method of analgesia for LLR as for OLR, while 3/5 of the centres used different methods of analgesia. Centres that used the same type of analgesia used mainly epidural (7/18) and PCA or opioid infusion (6/18). Centres that had changed the type of analgesia for LLR used mainly PCA or opioid infusion (18/27). Generally, PCA or opioid infusion was the most common type of analgesia, followed by epidural and intrathecal anesthesia. Regarding length of hospital stay (LOS), 30% reported LOS of <3 days, 44% between 4–6 days, 15% 7–9 days and 4% 10 days. Conclusion: Our survey shows evidence of varied perception of the intensity of postoperative pain following LHR and, consequently, variety in postoperative analgesia technique, which, contribute to different LOS. It has also shown the need for: 1) audits and 2) RCTs and improvement in communication and information exchange between centers about postoperative analgesia in LHR. | |
|
Keywords:
Analgesia, Laparoscopic, Liver resection, Postoperative
| |
|
Introduction
| ||||||
|
Since the first laparoscopic liver resection (LLR) in 1992, the global use of LLR has undergone an exponential increase [1] [2] [3]: a laparoscopic approach was chosen for approximately 30% of all liver resections and for more than 60% of left lateral segmentectomies performed at select centres worldwide [3]. Evidence indicates that LLR is associated with fewer complications, less blood loss, fewer transfusions, shorter hospital stays, equivalent operating times, and equivalent resection margins, especially for minor (left lobe) liver resections compared with open liver resection (OLR) (evidence of 2a) [4]. Although postoperative pain treatment plays an important role in enhanced recovery, little has been written about the type and duration of intraoperative and postoperative analgesia for LLR. Lower visual analogue scale (VAS) scores [5], a significant reduction in patient-controlled analgesia (PCA) use [6], and a shorter duration of analgesia [7] have been reported for LLR compared with OLR. However, little has been written about the type of postoperative analgesia, the role of multimodal analgesia, and the types of local anesthetics and opioids used. We performed an international audit in order to obtain the opinions of medical professionals involved in LLR about the postoperative pain intensity and use of postoperative analgesia in patients who have undergone LLR. | ||||||
|
Materials and Methods
| ||||||
|
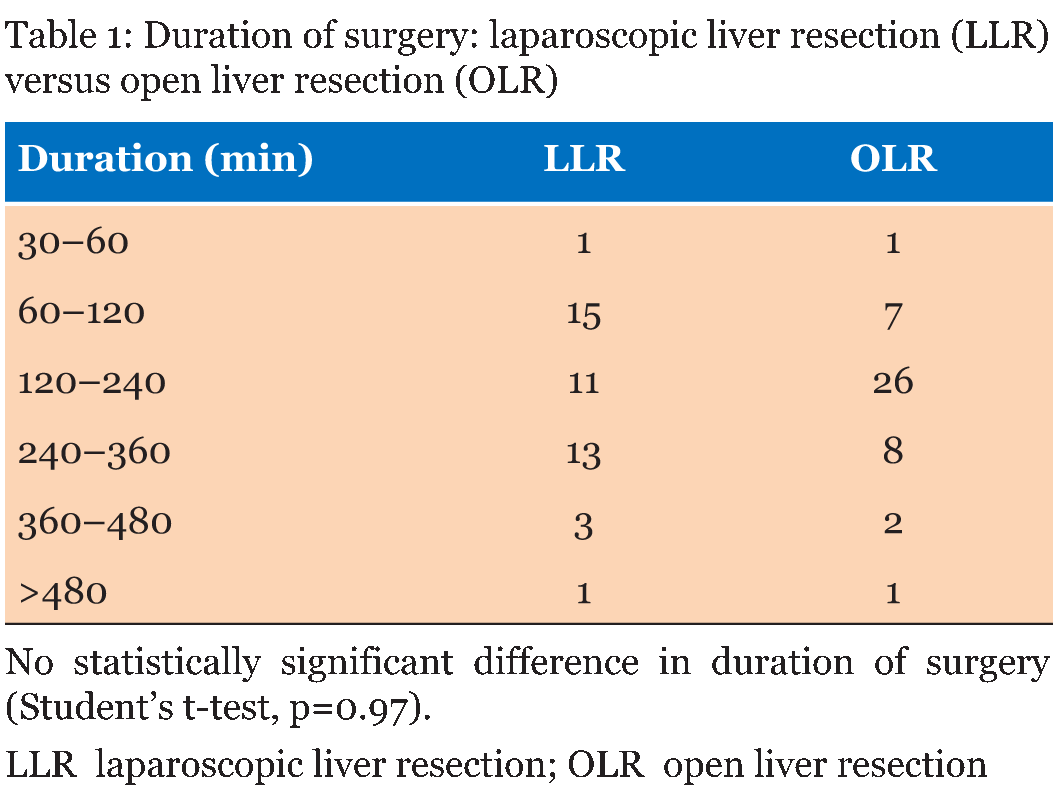
An online 24-question survey designed by us was sent to all centres with addresses on the International Liver Transplantation Society website (www.LiTAC.net). Additional questionnaires were sent to hepatobiliary units worldwide via personal contacts from our liver transplantation centre visitors and authors who had published reports on liver transplantation or liver resection. Of the 24 questions, 15 were multiple choice and 9 left space for answers. Data were collected over a six-month period, from September 2014 to March 2015. The results were collated using Google Docs and presented in Excel format and analysed by us. Data were presented in tables and graphics. We used Student's t-test to compare the difference in duration of surgery and the difference in the postoperative analgesia between laparoscopic and open liver resections. | ||||||
|
Results | ||||||
|
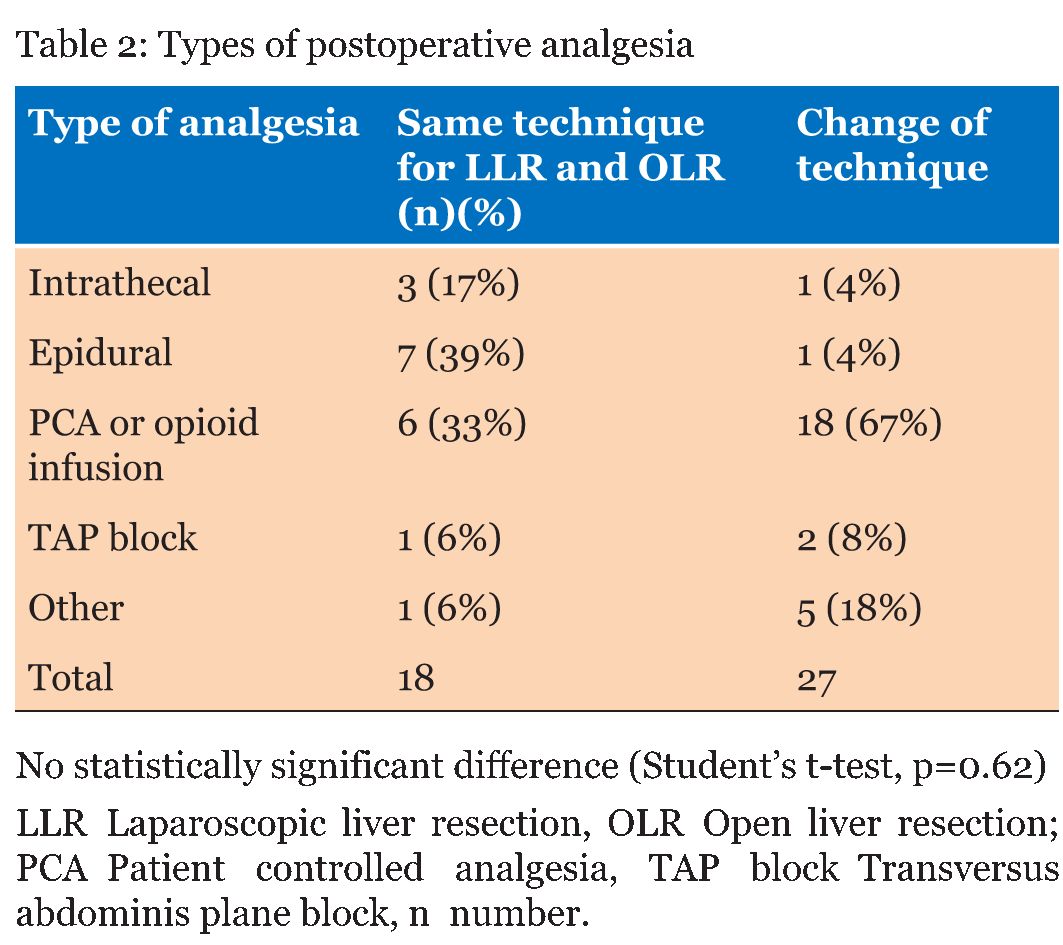
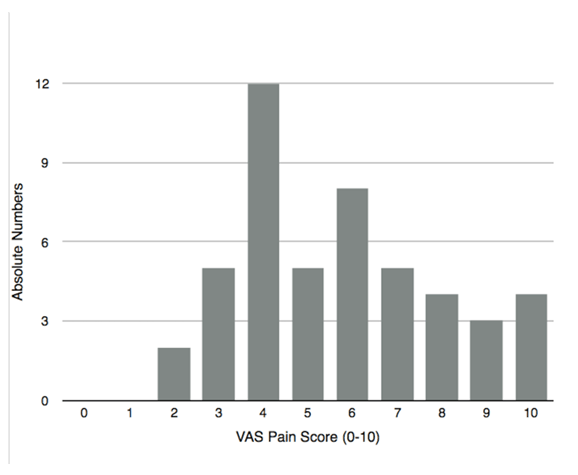
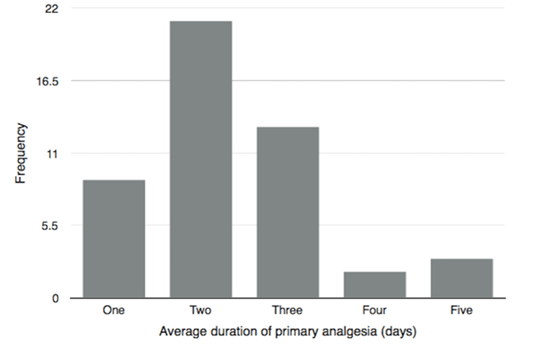
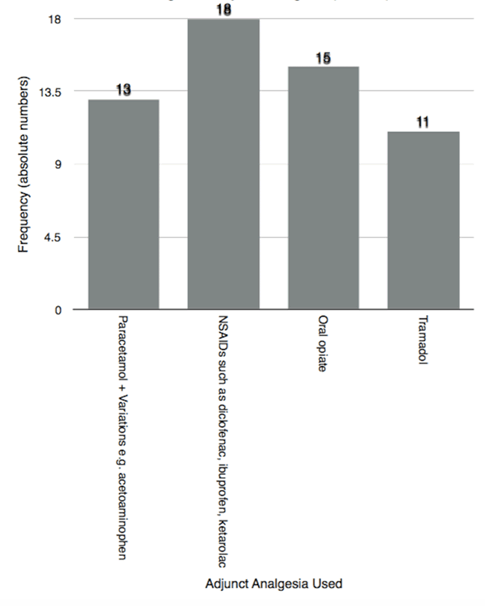
Of 158 questionnaires sent, 55 responses were received from 52 experts from centres, of which 45 performed LLR. We analyzed only the results from centres that performed LLR. The greatest number of responses came from Europe (n=22), followed by North/South America (n=13), and the Asia-Pacific region (n=11). Centre-related data Surgery-related data Pain intensity The estimated average pain scores (VAS 0–10) for laparoscopic procedures are shown in Figure 1. Only 2/45 respondents thought that the pain scores following LLR were lower than 2. Most of the responses (11/45) indicated VAS 4, while all of the scores above 4 were represented equally. Mode of primary analgesia Centres that used the same type of analgesia used the following types of analgesia: epidural (7/18), PCA or opioid infusion (6/18), intrathecal (3/18), and other analgesia (2/18). Centres that had changed the type of analgesia for LLR used mainly PCA or opioid infusion (18/27) and no epidural at all (Table 2). Patient controlled analgesia or opioid infusion was the most common type of analgesia, followed by epidural and intrathecal anaesthesia. There were no statistically significant difference in types of postoperative analgesia between centres that used the same technique and centres that changed technique of postoperative analgesia for LLR (Student's t-test, p=0.62) Intraoperative analgesia, type, and drugs used Duration of postoperative analgesia Who manages postoperative analgesia? Additional analgesia as a part of multimodal analgesia Transition from primary analgesia to the end of any analgesia Surgical local infiltration Length of hospital stay (LOS) | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
This international survey shows that in terms of postoperative analgesia following LLR:
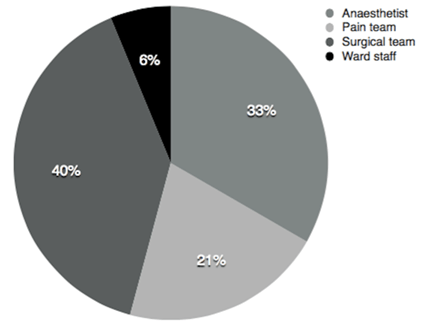
This survey also shows that anesthesia for hepatobiliary surgery is not a separate entity, and that anesthetists are not involved in the management of postoperative analgesia. Anesthetists are also not involved in publications on that topic. Thus, it is difficult to identify the anesthetists involved. The results of this survey are in accordance with those in literature in terms of the duration of LLR, intensity of pain, duration of analgesia, and LOS [8] [9] [10] [11] . Additional retrospective or prospective studies of analgesia in LLR are needed, including research on the effects of analgesia on recovery and tumur recurrence. Anesthetists should join with experts involved in LLR and contribute to postoperative pain treatment. The importance of this study is that it shows great variety in the way that postoperative analgesia is managed and it shows the need for more research in this area. There are a number of limitations to this survey. First, a small number of centres responded, despite significant effort and hundreds of e-mails sent. We received replies from both surgeons and anesthetists. Consequently, the details regarding analgesia were of different quality. Some parts of the world were not represented, including Africa, Egypt, and Turkey. Our efforts to find representatives were unsuccessful. The answers that we received and processed were based on the impressions of practicing surgeons and anesthetists and may not accurately represent the real situation. Most of the centres that submitted responses performed <50 LLRs/year. However, there are centres that perform >50 LLRs/year and the number of such centres is increasing [3]. The proportion of major liver resection is significantly higher in North/South America than in Asia-Pacific and Europe [3] . We received responses mostly from European centres. | ||||||
|
Conclusion
| ||||||
|
Our survey shows evidence of weak communication among anaesthetists involved in laparoscopic liver resection (LLR), varied perceptions of the intensity of postoperative pain following LLR, and variety in the postoperative analgesia techniques used, which, among other factors, contributes to differences in the length of hospital stay. It also shows a need for: 1) audits and 2) randomised controlled trials and improvements in communication and information exchange among centres regarding postoperative analgesia in LLR. Our contact database can become a platform for a website where anaesthetists can share their experiences. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Manu-Priya Sharma – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Georgina Cubas – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Simon Cottam – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published James Gill – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Gudrun Kunst – Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Zoka Milan – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Manu-Priya Sharma et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|