| Table of Contents |  |
|
Short Report
| ||||||
| Fast-tracking of adult patients following liver transplantation | ||||||
| Caroline Pocknall1, Jelena Marinkovic2, Zoka Milan3 | ||||||
|
1Anaesthetic ST6, Anaesthetic Department, King's College Hospital, London, UK.
2Professor of Statistics, Belgrade School of Medicine, Serbia. 3Consultant Anaesthetist, Honorary Senior Lecturer, Visiting Professor, King's College Hospital, London, UK. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Pocknall C, Marinkovic J, Milan Z. Fast-tracking of adult patients following liver transplantation. Edorium J Anesth 2016;2:6–9. |
|
Abstract
|
|
Introduction:
Fast-tracking of adult patients following liver transplantation has in the past been based on clinical decision making. A recent comprehensive scoring system from a single centre has a successful fast-tracking probability score of up to 92%. At our institution we used the same scoring system for research, to identify those patients who might be suitable for fast-tracking after liver transplantation and correlated their score with actual duration of postoperative mechanical ventilation and their preoperative (CPET) cardiopulmonary exercise testing scores.
Short Report: A retrospective audit of 30 consecutive adult patients undergoing liver transplantation was carried out over a 3- month period. Patients in acute liver failure and those who were ventilated preoperatively were excluded. A score for each patient was calculated based on age, gender, body mass index, MELD (model for end-stage liver disease) score, pretransplant length of stay, transplant number, intraoperative volume of red blood cell transfusion, operative time and vasopressor use in the last hour of surgery. Preoperative CPET scores were recorded along with duration of mechanical ventilation post-operatively. Thirty-three percent of the patients achieved a fast-track score associated with a successful predictor of fast-tracking, i.e., early extubation. These results showed a statistically significant association between fast-track score and actual time of postoperative mechanical ventilation. Preoperative CPET scores did not correlate with the fast-track score or duration of mechanical ventilation. Conclusion: A fast-track scoring system can be used to identify adult patients that are suitable for fast-tracking following liver transplantation surgery. This may reduce length of mechanical ventilation and ultimately reduce financial costs. | |
|
Keywords:
Early extubation, Fast-tracking, Liver, Transplantation
| |
|
Introduction
| ||||||
|
There is the evidence that fast-tracking liver transplant (LT) patients increase graft and patient survival [1]. Although fast-tracking in LT surgery has a long history, the decision to fast-track is based mainly on the clinician's experience [2] . Attempts have been made to base the fast-tracking decision on objective criteria [3]. Intraoperative blood loss, duration of surgery, use of inotropes at the end of surgery, and the last lactate level seem to be common factors in the decision to fast-track [3]. A recent comprehensive scoring system for fast-tracking has a probability of fast-tracking of up to 92% [1] . This scoring system is based on a single-centre experience that requires further validation [1]. Cardiopulmonary exercise testing (CPET) reflects preoperative cardiopulmonary reserve and is a sensitive and specific predictor of early survival after LT [4]. Seen also as a modifiable factor for improving patient survival following LT, it has never been evaluated as a contributing factor for fast-tracking LT patients [5]. Although we are a large transplant centre with excellent outcomes [6], we do not fast-track LT patients. The objective of this study was to identify what proportion of our patients might be eligible for fast-tracking. To confirm our findings, we also assessed the correlation between fast-tracking scores and duration of postoperative mechanical ventilation. Finally, we tested the value of the CPET results in the fast-tracking decision, by assessing the correlations between the CPET test results and fast-track scores and duration of postoperative mechanical ventilation (MV). | ||||||
|
Materials and Methods
| ||||||
|
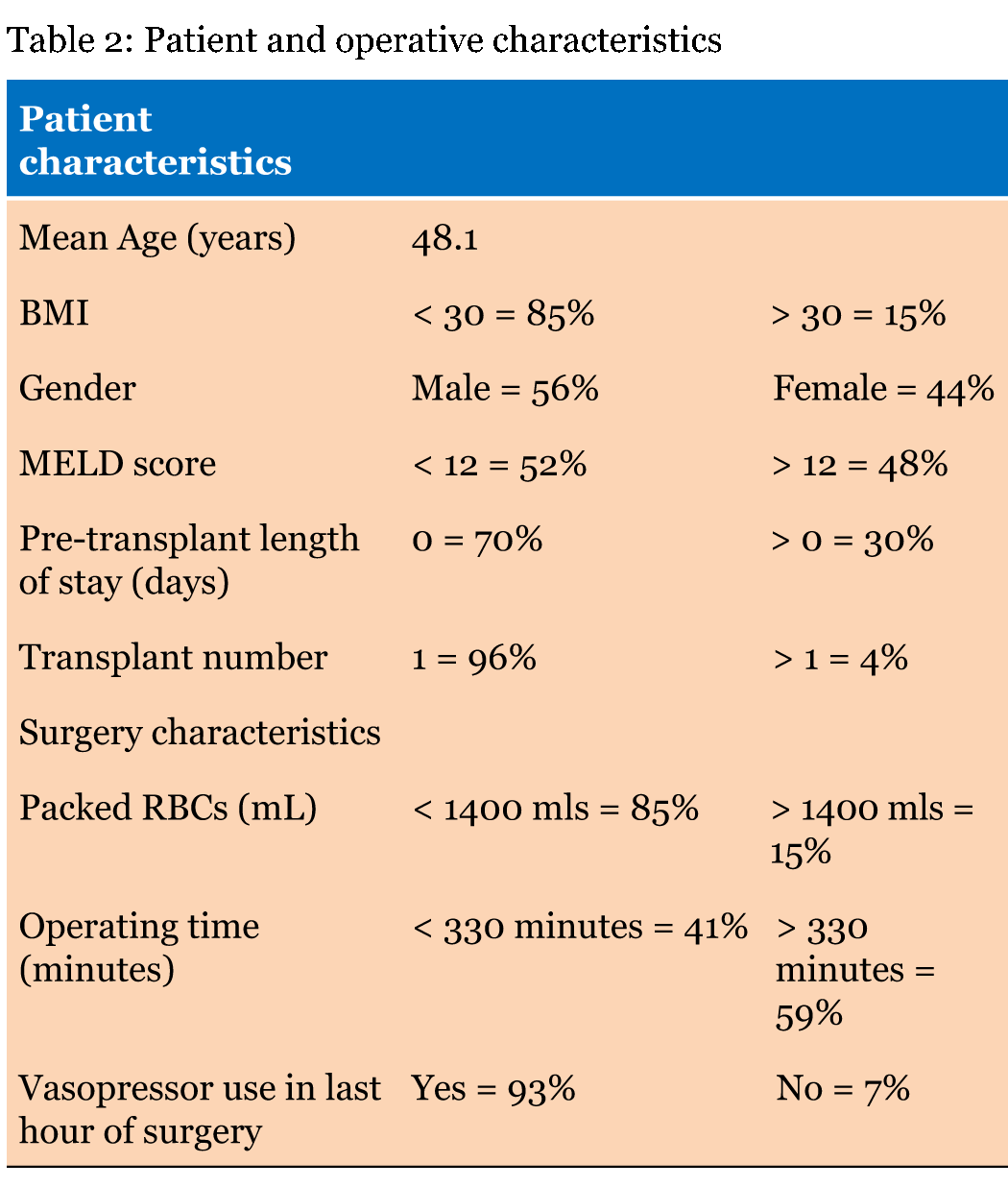
We retrospectively audited 30 consecutive patients who underwent LT between April 2015 and June 2015. We excluded three patients who had acute liver failure and were ventilated mechanically before LT. The standard anesthetic technique used in our hospital was used in all patients. We used intravenous midazolam 1–5 mg for brief sedation before inducing anesthesia with propofol or thiopentone 200 mg as the induction agent and fentanyl 100 µg and atracurium 50 mg to facilitate endotracheal intubation. To maintain anesthesia, we use isoflurane 1 MAC. We also used a continuous infusion of fentanyl 3–4 µg/kg/h for analgesia, atracurium 1 mg/kg/h for muscle relaxation, and noradrenaline as an inotrope, if required. Intraoperative monitoring included the oxygen saturation, invasive blood pressure, end-tidal CO2, anesthetic agent, central venous pressure, urine output, core temperature, Bispectral Index monitoring, and LiDCOrapid for hemodynamic monitoring. We retrospectively recorded the data presented in Table 1: age, gender, body mass index (BMI), model of end stage liver disease (MELD) score, pre-transplant length of stay, transplant number, red blood cell (RBC) transfusion, operating time, and vasopressor used in the last hour. All of these parameters are a part of the fast-tracking scoring system, which was not modified for our study. Individual scores were summed to obtain a fast-track probability score ranging from 0 to 13. The preoperative CPET findings were classified using anaerobic threshold and peak oxygen consumption to produce no (A), low (B), high (C), and very high (D) risk, as assessed by the professionals performing the CPET test. We also recorded the time until tracheal extubation following the completion of LT. We used univariate analysis of variance (ANOVA) to compare four groups and Spearman's correlation coefficient. | ||||||
| ||||||
|
| ||||||
| ||||||
|
Results | ||||||
|
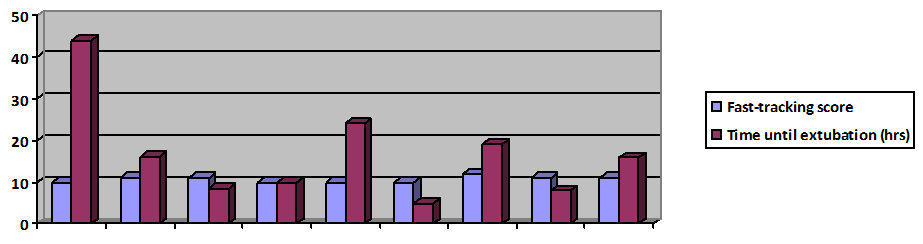
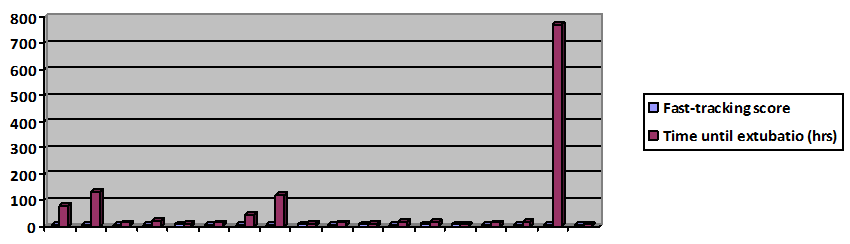
Of the 27 patients enrolled, 10 underwent LT for primary biliary cirrhosis/primary sclerosing cholangitis (PBC/PSC), five for alcoholic liver disease, five for metabolic disease, three for cirrhosis due to hepatitis C or B, three for cryptogenic plus non-alcoholic steatohepatitis, and one for a polycystic liver. Out of 27 patients, nine (33%) achieved a fast-track score of 10, predictive of successful early extubation (Figure 1). Another 16 patients (59.2%) had scores of 8 or 9, indicating 53% and 83% probability of fast tracking, respectively; based on work from the original study. Only two patients were not on inotropes at the end of surgery. The average duration of mechanical ventilation was 58.9 hours for all patients and 16.7 hours for the patients with a fast-track score of 10 or higher. There was a significant correlation between the fast-track score and duration of postoperative ventilation (–0.491, p=0.009). Based on the CPET data, 2/5 of the patients had low (A and B) perioperative risk and 3/5 had high (C and D) perioperative risk. The preoperative CPET data did not correlate with the fast-track scoring system or duration of mechanical ventilation. | ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
By auditing our small sample, we have shown that there is a great probability that at least one-third of the chronic liver disease patients in our institution are eligible for fast-tracking, and that another 60% could potentially be fast-tracked with small adjustments. Another 60% of our patients could have scores improved from 8 and 9 to 10 and 11 if they were off inotropes at the end of surgery. Our anesthetic technique includes continuous infusion of fentanyl and atracurium at the same dose or a dose slightly adjusted to the patients' needs throughout the surgery. The use of a shorter-acting anaesthetic and analgesic, or a decrease in the dosage of the currently used anesthetics following hepatic artery or even bile duct anastomosis would have led to a decrease in the dose or complete halt of the inotrope infusion at the end of surgery [7]. This audit also showed that the duration of surgery is another area of improvement that can lead to fast-tracking. A slight change in the proportions of the surgical work done by consultants and trainees could shorten the operating time to less than 330 min in more LT patients. Another area where improvement could have been achieved is blood and blood products replacement [8]. As the fast-track score had a negative correlation with the duration of postoperative mechanical ventilation, there is potential for reducing the length of mechanical ventilation and, consequently, the costs of care. The CPET test, representing patient fitness and exercise activity, assessed on a scale of 1–4, showed that we had more high-risk than low-risk patients and that there were no correlations of the CPET results with the fast-track score or duration of mechanical ventilation. | ||||||
|
Conclusion
| ||||||
|
This audit, conducted in our institution, showed that a fast-track scoring system can be used to identify adult patients that are suitable for fast-tracking following liver transplantation surgery. This may reduce length of mechanical ventilation and ultimately reduce financial costs. It may also be used as a tool for auditing current practice and detecting areas for improvement. The cardiopulmonary exercise testing (CPET) results, reported on a scale of 1–4, were not correlated with the fast-track scoring system or duration of postoperative mechanical ventilation. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Caroline Pocknall – Acquisition of data, Drafting the article, Final approval of the version to be published Jelena Marinkovic – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Zoka Milan – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Caroline Pocknall et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|