| Table of Contents |  |
|
Case Report
| ||||||
| Misleading elevation of the bispectral index (BIS) during return of neuromuscular activity | ||||||
| Pocknall Caroline1, Mihailovic Stevan2, Milan Zoka3 | ||||||
|
1ST6, Anaesthetic Department, King's College Hospital, London, UK.
2Consultant Anaesthetist, Specialist ofAnesthesiology, Reanimatology and intensive therapy, Opsta Bolnica Pancevo, Pancevo, Serbia. 3Consultant Anaesthetist, Honorary Senior Lecturer, Visiting Professor, King's College Hospital, London, UK. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Pocknall C, Mihailovic S, Milan Z. Misleading elevation of the bispectral index (BIS) during return of neuromuscular activity. Edorium J Anesth 2015;1:16–18. |
|
Abstract
|
|
Introduction:
The use of bispectral index (BIS) monitoring is now becoming standard practice for many anesthetists who feel it is a useful addition for measuring depth of anesthesia. We would like to highlight the limitations of interpreting BIS in the context of return of neuromuscular activity.
Case Report: A 67-year-old male undergoing general anesthesia for ablation of persistent atrial fibrillation with fentanyl and propofol TCI at effect site concentration 4 mg/ml; demonstrated a misleading elevation of the BIS value after return of neuromuscular activity evidenced by a cough reflex. After subsequent administration of a further dose of neuromuscular blocker, the BIS returned to its baseline value. The elevation of BIS towards a value consistent with a conscious state in our patient is confusing and is likely to be a reflection of alternative phenomenon such as the activation of the frontal electromyography (EMG) and interference with electroencephalographic (EEG) frequencies typical for wakefulness. Conclusion: The routine use of BIS monitoring needs to be evaluated in the context of other clinical parameters and awareness of interference from EMG activity and other mechanisms. | |
|
Keywords:
Bispectral Index monitoring, Anesthesia (General), Electromyography activity
| |
|
Introduction
| ||||||
|
The use of bispectral index (BIS) monitoring is becoming an integral part of standard practice for many anesthetists. It is a useful addition to the Association of Anesthetists of Great Britain and Ireland (AAGBI) monitoring standards, for measuring depth of anesthesia [1]. We would like to present a case report describing a misleading elevation of BIS value after provocation of a cough reflex, in a patient under general anesthesia. | ||||||
|
Case Report
| ||||||
|
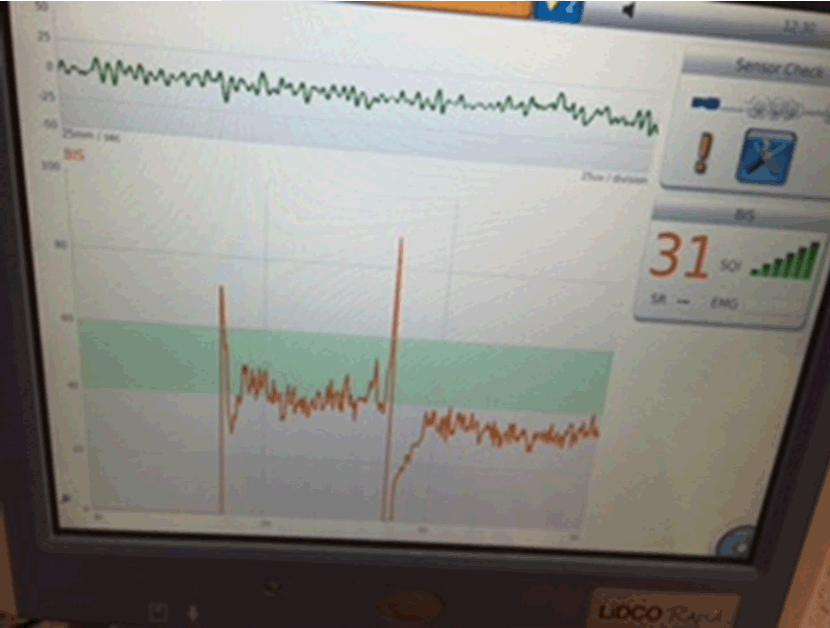
A 67-year-old male was undergoing general anesthesia for ablation of persistent atrial fibrillation. He was anesthetised with 100 micrograms of fentanyl and propofol target controlled infusion (TCI) at effect site concentration of 4 mg/ml. BIS monitoring as well as standard AAGBI monitoring was in place. From a baseline of 40–50, the BIS suddenly showed a spike to above 80 (Figure 1). This coincided with return of neuromuscular activity and cough reflex evident on the end-tidal carbon dioxide trace and an increase in airway pressures. After further administration of neuromuscular paralysis, BIS returned to its approximate baseline value. | ||||||
| ||||||
|
Discussion
| ||||||
|
As already known, the BIS index is a dimensionless value derived after analyzing raw, unprocessed electroencephalographic (EEG) activity as a reflection of brain electrical activity, and measured with frontal scalpe electrodes [2]. However, there are numerous clinical conditions, including electromyographic (EMG) activity, which could interfere with the spectrum of EEG frequencies analyzed by the BIS monitoring system algorithm, giving rise to the spurious picture of elevated activity of cerebral cortex, i.e., the brain arousal phenomenon [3] . The relative beta ratio; one of the parts of the proprietary BIS algorithm, records brain activity in the range of 30–47 Hz (low gamma range). These EEG waves could overlap with waves of the same frequencies (30–47 Hz) originating from the EMG activity of facial muscles, and thus be misinterpreted by the BIS monitoring system as EEG waves typical for cerebral arousal and possible awareness of the anesthetised patient [2][3]. Bruhn et al. reported two cases of falsely elevated BIS index value [4]. The authors concluded that the reason for the misleading increase of BIS was an elevation of electromyographic activity in the frontalis muscle and interference with the EEG waves of the same frequencies, probably as a result of opioid-induced muscle rigidity provoked by increasing effect site concentration of remifentanil. Baldesi et al. also reported a misleading elevation of the BIS index in a patient sheduled for surgery of acoustic neuroma, during which the EMG monitoring of facial nerve had been applied [5]. A cough reflex provoked during positioning of the patient's head coincided with an increase in BIS to 90. Increasing depth of anesthesia was unsuccessful in lowering BIS. A subsequent bolus of atracurium led to a decrease of the EMG activity, revealing a true BIS value of 30. Authors concluded that high frequency EMG waves from muscle activity weren't filtered by the BIS algorithm, which led to erroneous interpretation of those EMG waves as an high-frequency electroencephalography (EEG) waves indicating cerebral arousal. However, there may be other possible explanations for this increase in BIS produced by activation of muscle activity, which may have important clinical consequences. According to the Afferentation theory; the stretching of the primary and secondary endings of gamma motoneurons located within intrafusal muscle fibers of the muscle spindles, increases muscle afferent activity; which transmit neural impulses to the brain cortex and leads to cerebral stimulation and arousal. This is hemodynamically manifested as an increase in cerebral metabolic rate of oxygen consumption (CMRO2) and increase in cerebral blood flow (CBF), and electrophysiologically as an activation and "shifting" of EEG power spectrum towards higher frequencies. This hypothesis was elegantly tested in a classical study of Lanier et al. [6], who concluded that the activation of tracheal pain and mechanoreceptors (unmyelinated C-fibers and myelinated vagal afferents, respectively), led to the transmission of impulses to cerebral cortex and activation of neuronal activity. These findings suggest that coughing in a lightly anesthetized patient leading to phenomenon of cerebral activation and arousal could be explained by two mechanisms: Firstly, the activation of primary and secondary nerve endings within intrafusal muscle fibers, leading to an increase in muscle afferent activity and cerebral stimulation; the afferentation theory. Secondly, the cerebral activation could be induced by generating nerve impulses after stimulation of tracheal pain and mechanical receptors, and their transmission to higher brain centers in the cerebellum, somato-sensory and motor cortex. This, until recently, just a hypothetical idea was experimentally confirmed with functional MRI studies of the cough reflex, especially of the higher brain control centres and circuits [7][8]. These brain areas include primary sensory cortex, premotor and motor cortices, insular and prefrontal cortex, to name a few. This could have important clinical consequences, because preservation of activity of tracheal cough receptors in anesthetized patient, especially during "light" anesthesia, could stimulate those higher brain centers and give rise to the "shifting" of EEG frequencies toward the range typical for cerebral arousal. This could be missinterpreted by the BIS monitor as a patient wakefulness and lead to an inappropriate course of action. Also, we believe that the future versions of BIStm algorithm should include, if technically feasible, filtering of EEG frequencies characteristic for cerebral processing of coughing, as another source of interference with the function of BIS monitoring. | ||||||
|
Conclusion
| ||||||
|
The case report demonstrates that the elevation of bispectral index (BIS) towards a value consistent with a conscious state in our patient is likely to be a reflection of alternative phenomenon as opposed to an increase in electroencephalographic (EEG) activity secondary to noxious stimuli. The increase of BIS in the current report would probably be caused by the increase of electromyographic (EMG), however some other causes might be considered such as afferent theory or activation of the cerebral cortex during cough reflex. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Pocknall Caroline – Acquisition of data, Drafting the article, Final approval of the version to be published Mihailovic Stevan – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Milan Zoka – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Pocknall Caroline et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|