| Table of Contents |  |
|
Case Report
| ||||||
| Difficult venous access in a child with a severe form of scleromyxedema | ||||||
| Biljana Drašković1, Dragan Marinković2, Fabri Izabella3 | ||||||
|
1Professor of Anesthesiology, Anesthesiologist, Department of Surgery, Medical Faculty, University of Novi Sad, Serbia Anesthesiologist, Head of Department, Department of Anesthesia, Intensive Care Medicine and Pain Therapy, Clinic of Pediatric Surgery, Institute of Healthcare of Children and Youth of Vojvodina, Novi Sad, Serbia.
2Anesthesiologist, Department of Anesthesia, Intensive Care Medicine and Pain Therapy, Clinic of Pediatric Surgery, Institute of Healthcare of Children and Youth of Vojvodina, Novi Sad, Serbia. 3Teaching Assistant of Anesthesia, Department of Surgery, Medical Faculty, University of Novi Sad, Serbia. Anesthesiologist, Department of Anesthesia, Intensive Care Medicine and Pain Therapy, Clinic of Pediatric Surgery, Institute of Healthcare of Children and Youth of Vojvodina, Novi Sad, Serbia. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Drašković B, Marinkovic D, Izabella F. Difficult venous access in a child with a severe form of scleromyxedema. Edorium J Anesth 2015;1:6–9. |
|
Abstract
|
|
Introduction:
Scleromyxedema, is a very rear condition of mucinous deposition and diffuse papular eruptions of the skin, accompanied by systemic complications.
Case Report: A case of a 12 years old boy whose disease first presented with multiple painful aphtous ulcers in his mouth, papular skin eruptions on his palms and soles and hyperthermia up to 38.3°C. Over a period of four years the disease advanced progressively with rapid spreading of the skin lesions on the boys extremities, trunk and neck. On our first contact with the patient, he was in a very altered health condition, severely underfed, almost paralized with rigid flexion of all of his proximal and distal joints. His skin was thick and unpenetrable, intravenous cannulation and administration of therapy, laboratory testing was impossible. Neck extension and mouth opening were severely limited. The positioning for central vein puncturing was impossible and therefore it was decided to place a central venous catheter under the control of ultrasound. The procedure took place in the operating theatre, under analgosedation with Chloral hydrate administered rectally and N2O/air mixture through a facial mask. The right internal jugular vein was cannulated using the out-of-plain technique, with a 18G catheter under the guidance of a 6 cm linear ultrasound probe. Conclusion: The procedure was successful with no intra- or postoperative complications. Ultrasound guided central vein insertion appeared to be of a major significance in this case of a very difficult vascular access, presenting as a safe, easy and lifesaving technique. | |
|
Keywords:
Central venous catheters, Scleromyxedema, Ultrasonography
| |
|
Introduction
| ||||||
|
Scleromyxedema involves mucinous deposition in the skin and is associated with the presence of monoclonal gammopathy, characterized by a papular skin eruption. This illness has not been previously reported in children [1]. We report herein a case of a 12-year-old male suffering from a severe form of scleroderma who presented for central venous access. | ||||||
|
Case Report
| ||||||
|
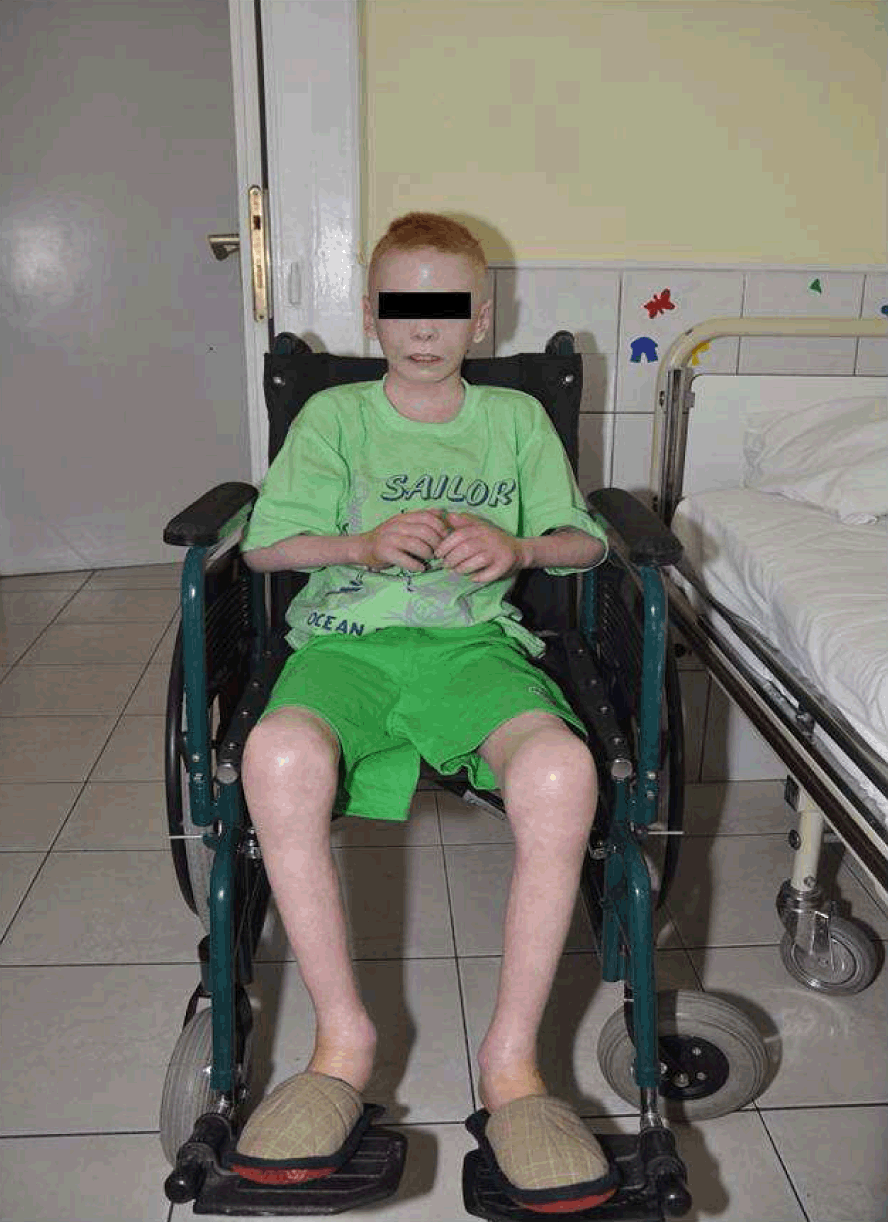
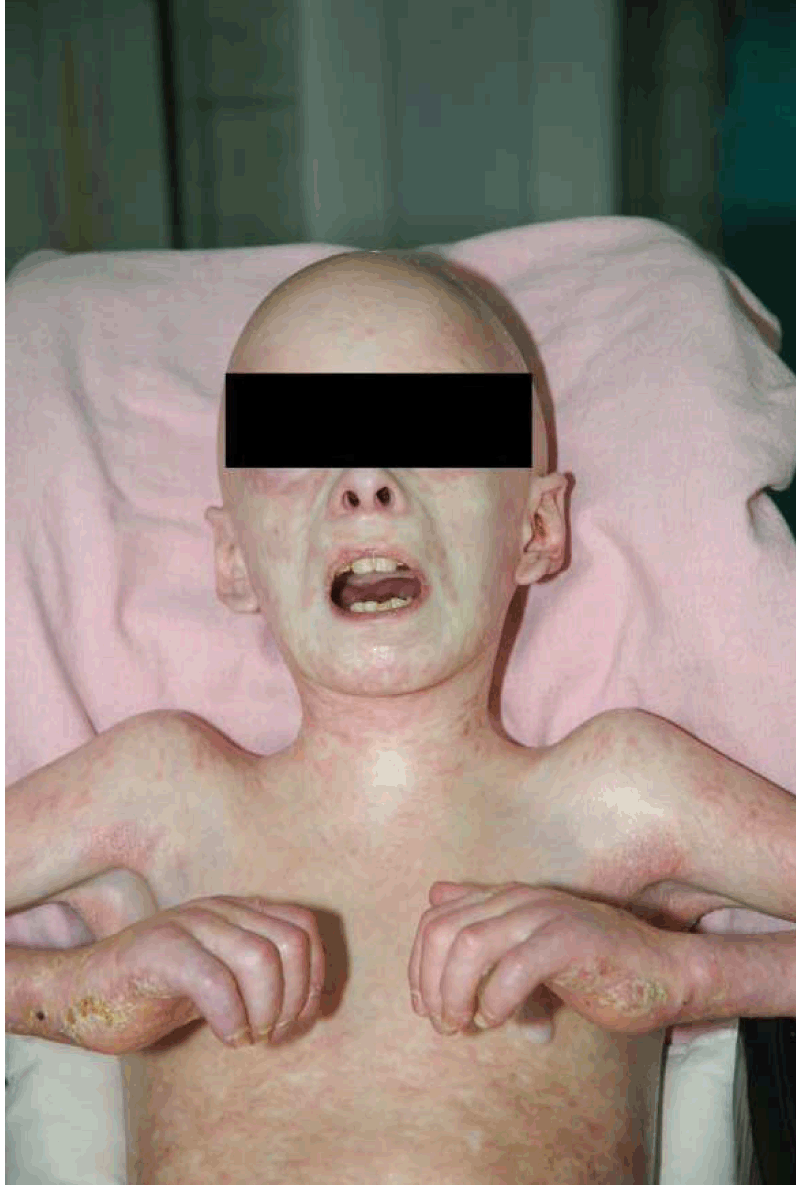
The patient was a wheelchair-bound 12-year-old male with severely limited movement amplitudes and rigid flexion of all joints. His skin was covered with diffuse adherent sclerotic plaques, and he exhibited limited neck extension and mouth-opening. The patient's tongue was hyperemic and edematous with aphthous ulcers. The patient was also severely underfed (Figure 1). The severely compromised condition of the patient required the use of a central venous catheter. Considering his condition, ultrasound-guided access in the operating theater under sedation and analgesia appeared acceptable. However, the impossibility of medicating by venous access or by the oral route required us to take a different approach to sedation (Figure 2). Chloral hydrate was administered rectally for sedation purposes at a dose of 100 mg/kg. The patient was placed on the table in the left lateral position. He was breathing spontaneously via a face mask with a mixture of 40% N2O and 60% O2. Using aseptic techniques, the right internal jugular vein was viewed using a linear, 6–10 MHz 8L RS, GE Logiq Book XP ultrasound probe (GE, Fairfield, CT, USA). An 18-gauge catheter (CertofixÓ Mono; B. Braun Medical Ltd., Sheffield, UK) was inserted into the right internal jugular vein using an out-of-plane approach and application of the Seldinger technique. The procedure ended safely with no complications. The central venous catheter was secured and flushed according to standard protocols for central venous catheter management. The central venous catheter enabled easy blood sampling and, together with rebiopsies of the skin, accurate diagnosis. It was also possible to administer the intended immunomodulatory biological therapy and supplementary parenteral nutrition. | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Scleromyxedema is a chronic and occasionally fatal systemic disease [2]. Although the etiology of scleromyxedema remains unclear, 80% of patients exhibit a paraprotein, typically IgG lambda, which represents an immunologic trigger for the deposition of mucin [3]. Histological findings reveal three key features: interstitial mucin deposition, thickened collagen bundles, and an increased number of fibrocytes [1]. Diagnosis in our patient was extremely difficult because the clinical symptoms resembled numerous clinical features of the so-called scleroderma mimics [3]. Until now, scleromyxedema had not been described in children. In our case, the disease first presented with thickened skin on the upper extremities. The patient also had sclerodactyly, esophageal dysmotility with resultant dysphagia, joint pain, decreased mobility, and joint contractures, which are among the most common features of the disease [1] [3]. Even though scleromyxedema commonly affects the nervous system and causes a dermato-neuro syndrome, our patient was psychically stable with proper affective reactions despite his poor condition [1] [2]. The patient also had restrictive respiratory function, subclinical hypothyroidism, osteoporosis, and hypertrophic cardiomyopathy with mitral valve dysplasia, which are among the most common systemic complications of the disease. Vascular cannulation procedures in children are highly delicate and have been associated with numerous complications. Our patient was admitted to the ward due to the impossibility of venous cannulation and consecutive laboratory testing. It was not possible to place him in the position typically used for conventional cannulation of the internal jugular vein. Positioning the patient such that his neck was bent and his extremities were in the left lateral position was the only way to achieve a moderately acceptable position for the cannulation procedure. The patient's limited ability to open his mouth, poor visibility of pharyngeal structures, and an inter-incisor distance of < 2 cm indicated extremely difficult airway access. A chest X-ray indicated atelectatic lung fields, and respiratory functional tests revealed a significant restrictive respiratory disorder. This led to the decision to avoid general anesthesia. The use of ultrasound guidance for central venous cannulation has been recommended for pediatric patients and in cases with difficult central venous access. Cannulation of the internal jugular vein can be performed using either the in- or out-of-plane technique [4]. We decided to cannulate the vein using an out-of-plane approach, under real-time ultrasound control, as this was the technique with which we were most familiar. To avoid general anesthesia, the patient was sedated with chloral hydrate and analgesia was provided with a mixture of N2O/air administered via a face mask while he breathed spontaneously. The use of ultrasound guidance for central venous cannulation reduces the number of puncture attempts, thereby reducing the risk of puncture-related complications and catheter-associated infections [4] [5]. The cannulation procedure in our case proceeded smoothly with no complications. To date, the patient has received four central venous catheters, which all remained in place for > 30 days with no signs of infection or any other complication that may be associated with the use of these invasive devices. | ||||||
|
Conclusion
| ||||||
|
This case was unique in several ways, including because severe scleroderma in a child has not been described previously. The patient's altered mobility, restricted pulmonary function, and cardiomyopathy limited our anesthetic and therapeutic options. Due to good planning of analog sedation and ultrasound-guided central venous access, the procedure went smoothly. Central venous catheterization facilitated intravenous treatment, blood sampling, and parenteral nutrition. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Biljana Drašković – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Dragan Marinković – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Fabri Izabella – Substantial contributions to conception and design, Acquisition of data, Analysis an interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Biljana Drašković et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|